Minimize Scarring: How to Care for a Facial Wound From Start to Finish
In July 2020, my good friend Thurman was riding an electric scooter when he hit a pothole and flew over the handlebars. He happened to be in Austin working on Tankproof, his nonprofit organization (of which my company is a huge supporter!). He FaceTimed me from the emergency room and wow, his face really got torn up badly. Now, over a year later, his wounds are thankfully healed up and I’ve been helping him deal with the scar left behind. Scars are a really challenging skin concern because they’re formed so deeply within the skin. I’ve written about different types of acne scars, but for this post, I wanted to address scars caused by an injury in hopes it could help you if you should find yourself in this type of situation.Â
When you injure yourself, whether or not a scar forms isn’t always within your control (and getting your injury seen by medical professionals is always the first priority). That said, by sharing Thurman’s story, I’ll talk about what you can do to minimize scarring from a wound at various stages of healing. I’ll also share additional insights from Dr. Sam Lam, a board-certified facial plastic surgeon at Lam Facial Plastics, who has been helping advise Thurman on how to reduce scarring and hyperpigmentation.
Phase 1: In the ER
When Thurman FaceTimed me from the emergency room right after his accident, I happened to be having dinner with a friend of mine who is an ER doctor. He walked Thurman through what he could expect in terms of general wound care and stitches and told him to ask if there was a cosmetic surgeon on call in the ER. Luckily, there was! They numbed his face before thoroughly cleaning out his wound then stitching it up.
After he got back home to Baton Rouge, Thurman made an appointment with a local plastic surgeon to have the stitches checked out and make sure everything was in order. Dr. Lam agreed that this was a good move—once your injuries have been taken care of and you’re in the clear, you can turn your attention to aesthetics.
“When you have an open wound,†says Dr. Lam, “the first thing is to get it cared for and stitched up as quickly as possible. The longer it sits open, the greater the risk of infection. After this, I would advise beginning a relationship with a plastic surgeon who can help you manage the healing process to reduce scarring and hopefully avoid the need for future scar revision.â€
Phase 2: Caring for the Wound to Minimize Future Scarring
For the first few weeks after getting stitched up, your priority should be caring for your wound according to your doctor’s instructions. Following their advice diligently is one of the best things you can do to minimize future scarring.Â
“The main thing was keeping it clean,†Thurman says. “They also had me apply antibiotic ointment to keep it moist.â€
Ointments used for wound care are usually petrolatum-based, which means they’re also very thick and occlusive. This allows them to form a protective seal over the skin. While this is ideal for healing, in some cases it can lead to enlarged or clogged pores. 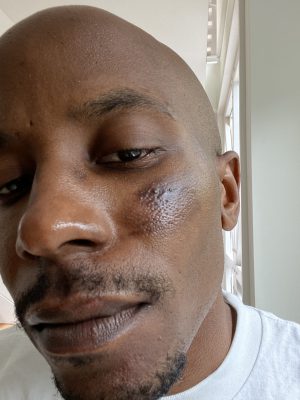
This is what happened to Thurman, who developed a few milia on his cheekbone (you can see one of the bumps in the photo on the right). Milia are small, hard bumps that form within pores as a result of keratin becoming trapped beneath the surface of the skin. I believe Thurman’s scar tissue was especially vulnerable to this because it was basically raw tissue, and the pores were being re-formed. The thick ointment kept some of these new pores expanded as did the location of the scar—our cheeks are stretched a lot from facial movements such as smiling and talking.Â
Once Thurman’s wound had started to heal and was no longer raw, I performed extractions to remove the milia for him. I also had him get a prescription retinoid and confirm with a dermatologist that it was safe to start using it on his scar. He continues to use it twice a week to help shrink the appearance of enlarged pores.
Dr. Lam’s Recommendations
Per Dr. Lam’s suggestion, Thurman had also started using silicone patches to cover his scar and improve its appearance. Silicone patches can minimize scarring by increasing the hydration within the outer layers of the skin. This can also help regulate collagen production, which may result in a flatter scar. Additionally, silicone patches can help keep scar tissue protected by shielding it from bacteria.Â
During the early stages of healing, Dr. Lam notes that he also likes to have patients use hypochlorous acid: “I love medical-grade hypochlorous acid. It allows wounds to heal well by reducing bacteria and other contaminants, and it naturally minimizes contamination without risk to the tissue integrity.â€
Be sure to consult with your doctor before using anything at home to make sure it’s a good fit for your wound.
Phase 3: The Scar Settles, and Hyperpigmentation Sets In
Once the skin heals and a scar is no longer fresh, one of two things can happen to your skin’s pigment: the first is hyperpigmentation, and the second is hypopigmentation.
Hyperpigmentation refers to areas of skin that become darker than your natural skin tone as a result of trauma or overstimulation. In response to an injury, your skin’s melanocytes (the cells that give our skin its color) are activated. In some cases, they become a little overzealous in their healing response and end up creating more pigment than they’re supposed to. This is why acne leaves marks behind.
Hypopigmentation, on the other hand, is exactly the opposite. An injury damages melanocytes and causes them to die off, resulting in a loss of pigment. This is why some scars turn white after they heal. This loss of pigment is incredibly hard to reverse, but there are some laser-resurfacing procedures that may be able to improve it.Â
Managing Thurman’s Hyperpigmentation
At this point, Thurman’s wound was completely closed up and hyperpigmentation had set in (his scar had turned dark). Hyperpigmentation was something we needed to be particularly aware of with Thurman because of his skin tone. The deeper your skin tone, the more active your melanocytes are. If melanocytes are more active, to begin with, there’s an even greater risk for hyperpigmentation as the result of injury or trauma. It can also be a lot harder to reverse hyperpigmentation since melanin activity is harder to suppress, so I really encouraged Thurman to stay on top of this from the beginning.
Sun Protection
The first and most important aspect of this was keeping the scar protected from the sun. The whole goal is to get melanocytes to calm down and to signal to them that the skin is no longer under threat. UV light is a major trigger for hyperpigmentation because it stimulates melanocytes, so keeping sensitive scar tissue protected from the sun is a must. Of course, I made sure Thurman was properly applying sunscreen to his face and neck, taking extra care to cover his scar. Additionally, I believe it helped that he was still wearing a protective face mask much of the time. (Maskne may be a real nuisance, but the extra sun protection can be a bonus!)
Topical Vitamin C
Vitamin C is a powerful antioxidant that can offer additional protection against UV rays when paired with sunscreen. I had Thurman use the Renée Rouleau Vitamin C & E Treatment because it uses a form of vitamin C called tetrahexyldecyl ascorbate. This is a very effective, fat-soluble version of vitamin C that has to be converted by the skin’s own enzymes, making it much gentler than L-ascorbic acid. Since scar tissue is very sensitive, I didn’t want Thurman putting something that acidic on it every morning before applying his sunscreen.
Exfoliation
For this reason, I also didn’t have Thurman start to exfoliate until after all of the fresh, pink scar tissue had healed and transitioned to hyperpigmentation. At this point, I had him add the Renée Rouleau Pore + Wrinkle Perfecting Serum into his routine one to two nights a week.Â
Phase 4: Professional Treatments
One of Dr. Lam’s preferred treatments for scars is Botox injections.Â
“To me, Botox is the most incredible healing agent,†he says. “In double-blind placebo-controlled studies, even a few units of Botox placed a week after a scar has been shown to help with healing. I like to do it soon after surgery or stitches, but honestly anytime in the first six months is helpful. The sooner the better.â€
When Thurman reached out to Dr. Lam about ways to improve the appearance of his scar, Dr. Lam cautioned against anything too invasive for fear of either creating more hyperpigmentation or, worse, permanently depigmenting the area. He recommended Botox as a less invasive alternative, and Thurman plans to try it out.Â
Surgical Interventions
According to Dr. Lam, it takes most scars a year to fully mature. Depending on the severity, a lot of them will improve on their own. This is why Dr. Lam advises waiting a year before considering surgical intervention. If you’re still unhappy with the appearance of your scar at this point, he says there are a number of procedures that can address different aspects of scarring, from irregular pigmentation to raised or uneven borders. His advice is to find an experienced surgeon with good reviews and many years of practice who also has extensive before and afters that you like. From there, your surgeon will be able to advise you on the best procedure for your scar type.
Conclusion
As you can see, managing a scar is a long and tedious road. Certain scars are inevitable but know there are steps you can take to minimize their appearance and if they still bother you, procedures and treatments that can improve them later on.Â
As for Thurman, he says he’s happy with the way things played out and notes that being kind to yourself is important when dealing with any kind of recovery from injury.
“There are definitely psychological struggles that accompany it,†he says, “and they kind of ebb and flow. My advice to anyone going through a similar situation or healing process is just to be patient and be kind to yourself.â€
The post Minimize Scarring: How to Care for a Facial Wound From Start to Finish appeared first on Expert Skin Advice from Renee Rouleau.






![The 7 Most Important Nutrients For Healthy Skin [Inforgraphic] 8 The 7 Most Important Nutrients For Healthy Skin [Inforgraphic] 8](https://freshnaturalskin.com/wp-content/uploads/2021/12/face-oil-520x245.jpg)


